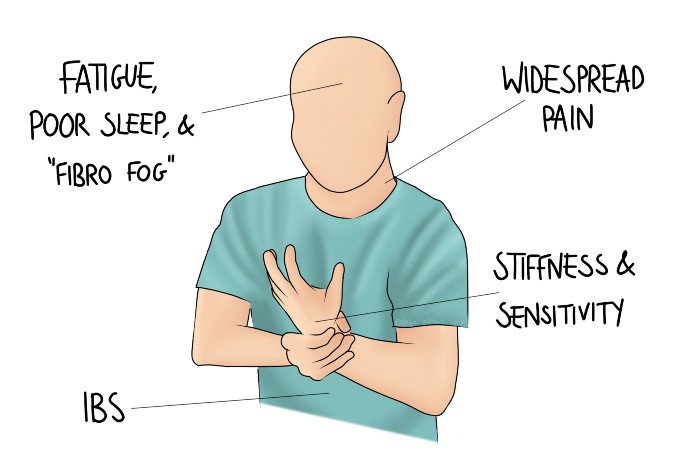
Fibromyalgia is a condition that causes widespread pain and tenderness in the body. It can also cause sleep disturbance and difficulty concentrating (“brain fog” or “fibro-fog”).
Symptoms of Fibromyalgia
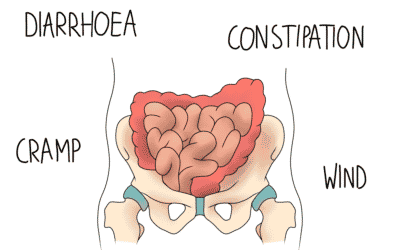
Fibromyalgia is a condition of widespread, chronic pain. By definition, chronic pain lasts over three months. Some people have pain all over their body, whereas others may be spared a limb or two. Alongside the pain, the condition can be recognised by its joint stiffness and fibro-fog. Associated conditions include migraine and IBS.
Frustratingly, fibromyalgia is hard to define. There are no diagnostic tests for it- it is diagnosed by the absence of another diagnosis. It used to be diagnosed by the presence of tender points at specific spots in the body, but this method of diagnosis has been disproven. Signs will not show on MRI or X-Ray, as this is a functional condition. Now it is generally diagnosed by ruling out other causes.
Managing Fibromyalgia
Fibromyalgia is now considered to be an error in pain processing. One element of this is sensitisation. Here pain is felt from stimuli that shouldn’t normally be painful (allodynia). Painful stimuli may also cause more pain than normal (hyperalgesia). Sensitisation may respond well to a mix of avoidance and exposure. By avoiding the things that aggravate the pain, the nervous system may be able to calm down a bit. Then exposure to those stimuli can be gradually built up, teaching the brain that these things are not a threat. The most basic role of pain is to protect us.
Avoidance may be difficult when the cause of the pain is more widespread. However, if you know that certain activities do make your symptoms worse, we may be able to work with that. Exposure may be more relevant here. If your pain responds to this kind of management, we might find that gradually building your activities back up works for you.
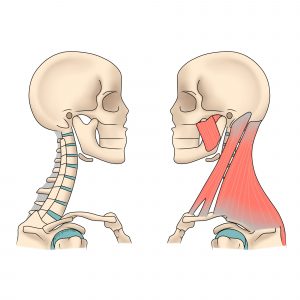
A good management strategy will address the pain processing side of things. Your osteopath may also want to work elsewhere in the body if they think that there’s an element of overloading or compensation playing a part. One of the body’s favourite protective mechanisms for pain is to tighten up the local muscles in an effort to prevent further damage. There is no damage in this case, so relaxing off these muscles might help.
Similar Conditions
ME and Chronic Fatigue Syndrome (CFS)
These two conditions are closely related to fibromyalgia. All are functional illnesses that cause tiredness, difficulty concentrating, and reduced capacity for activity. ME/CFS may also come with pain. All symptoms can come and go, and don’t necessarily follow a pattern.
Long Covid
Some people think that the onset of fibromyalgia may be a viral infection. Long Covid is essentially a form of post-viral fatigue, and there are similarities to draw with fibromyalgia (and ME/CFS) too. This complication tends to affect people who had milder symptoms, but not exclusively. As the symptoms of COVID ease, the long Covid symptoms appear, or become more apparent. Low energy, muscle aches, and brain fog are the primary symptoms. The science is still emerging, but the general recommended approach has been multi-disciplinary. Osteopathy may have a role to play in improving breathing mechanics, or helping with joint and muscle pain.
Start managing your fibromyalgia now: book an appointment here.